
Welcome to New Hope Physiotherapy
- Brampton 905-846-4000
- Malton 905-364-3900
- Orangeville 519-217-9300
- admin@newhopephysio.com
- Home
- Blog
Common Pelvic Floor Issues and How Physiotherapy Can Help
 11 Jun 2023
11 Jun 2023
- Comments
- 724
Common Pelvic Floor Issues and How Physiotherapy Can Help
Pelvic floor issues are more common than you might think, affecting individuals of all ages and genders. These issues can have a significant impact on one’s quality of life, causing discomfort and disrupting daily activities. Thankfully, physiotherapy offers effective solutions for treating and managing pelvic floor problems. In this blog post, we will explore some common pelvic floor issues and discuss how physiotherapy can help alleviate symptoms and improve overall well-being.
Also Read: World Arthritis Day 2025: Raising Awareness About Joint Pain
1. Urinary Incontinence
Urinary incontinence is a common pelvic floor issue that affects both men and women, although it is more prevalent among women. It can manifest in different forms, such as stress incontinence, urge incontinence, or a combination of both.
A. Stress Incontinence
This type of incontinence occurs when there is pressure on the bladder, leading to leakage during activities such as coughing, sneezing, laughing, or exercising. It is commonly caused by weakened pelvic floor muscles and a loss of bladder support. Pregnancy, childbirth, menopause, and certain medical conditions can contribute to stress incontinence.
B. Urge Incontinence
Also known as an overactive bladder, urge incontinence is characterized by a sudden, intense urge to urinate, followed by an involuntary loss of urine. It occurs due to involuntary contractions of the bladder muscles, causing an urgent need to urinate. In some cases, the cause of urge incontinence is unknown, but it can also be related to neurological conditions or bladder irritants.
Physiotherapy for Urinary Incontinence
Physiotherapy offers a non-invasive and conservative approach to managing urinary incontinence. It focuses on strengthening the pelvic floor muscles, improving bladder control, and modifying lifestyle factors that contribute to incontinence. Here are some techniques commonly used in physiotherapy for urinary incontinence:
A. Pelvic Floor Muscle Exercises (Kegels)
These exercises target the muscles that support the bladder, urethra, and other pelvic organs. A physiotherapist can guide you on proper technique and provide a personalized exercise program based on your specific needs. Regular practice of pelvic floor muscle exercises can help strengthen the muscles, enhance urinary control, and reduce leakage.
B. Biofeedback
Biofeedback is a technique used to help individuals become aware of their pelvic floor muscles and learn how to control them effectively. It involves using specialized equipment or sensors to provide visual or auditory feedback on muscle activity. By receiving real-time information about muscle contractions, individuals can learn to engage and relax the pelvic floor muscles correctly.
C. Bladder Training
Bladder training aims to improve the bladder’s capacity and control the urge to urinate. A physiotherapist can help develop a personalized bladder training program that involves gradually increasing the time between voids and learning strategies to suppress the urge to urinate. Over time, this can help improve bladder control and reduce episodes of urinary incontinence.
D. Lifestyle Modifications
Certain lifestyle factors can contribute to urinary incontinence. Your physiotherapist can provide guidance on dietary adjustments, fluid intake management, and strategies to avoid bladder irritants like caffeine and alcohol. They may also suggest adopting healthy toileting habits and techniques to empty the bladder fully.
E. Electrical Stimulation
In some cases, physiotherapists may use electrical stimulation as an adjunct therapy for urinary incontinence. This technique involves the use of a device that delivers electrical impulses to the pelvic floor muscles, helping to strengthen and re-educate them. It can be particularly beneficial for individuals who have difficulty activating their pelvic floor muscles voluntarily.
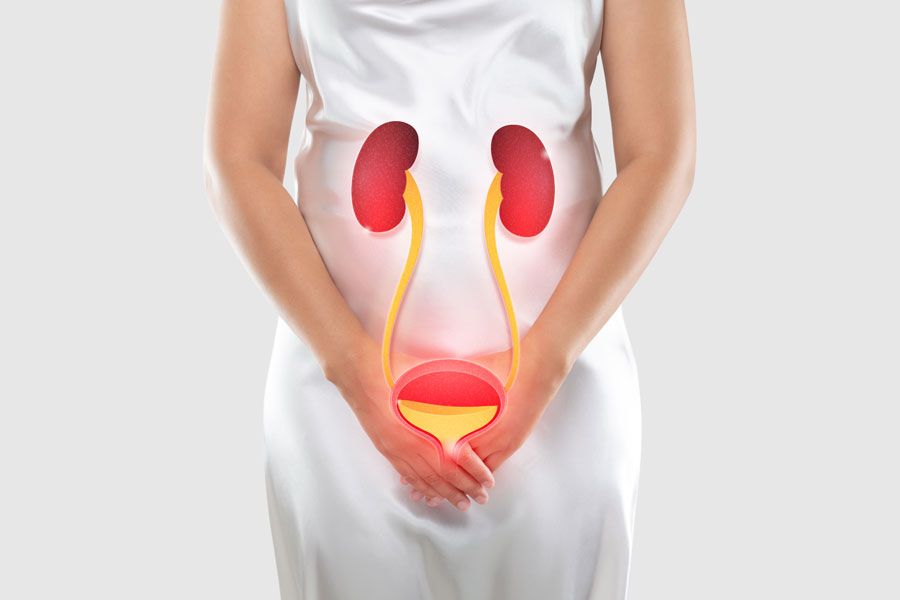
Remember, every individual is unique, and the treatment approach for urinary incontinence may vary. It’s essential to consult a qualified physiotherapist who specializes in pelvic floor rehabilitation. With their expertise and guidance, you can regain control over your bladder and enjoy a more active, comfortable lifestyle, free from the constraints of urinary incontinence.
2. Pelvic Organ Prolapse
Pelvic organ prolapse is a condition that occurs when the pelvic organs, such as the bladder, uterus, or rectum, descend from their normal position and bulge into the vaginal canal. It is often caused by weakened or damaged pelvic floor muscles and ligaments that are responsible for supporting these organs. Pelvic organ prolapse can lead to various symptoms depending on the organs involved, including a sensation of pelvic pressure, urinary difficulties, bowel problems, and discomfort during sexual intercourse.
Also Read: World Mental Health Day 2025 – New Hope Physiotherapy
Types of Pelvic Organ Prolapse
A. Cystocele
A cystocele occurs when the bladder prolapses into the vaginal canal. This can lead to urinary symptoms such as frequent urination, urgency, incomplete emptying, and stress urinary incontinence.
B. Rectocele
A rectocele involves the bulging of the rectum into the back wall of the vagina. It can cause difficulty with bowel movements, a sensation of incomplete emptying, and even constipation.
C. Uterine Prolapse
Uterine prolapse occurs when the uterus descends into the vaginal canal. This can result in a feeling of pelvic pressure, discomfort, and sometimes urinary or bowel symptoms.
D. Vaginal Vault Prolapse
This type of prolapse can occur after a hysterectomy when the top of the vagina descends into the vaginal canal.
Physiotherapy for Pelvic Organ Prolapse
Physiotherapy plays a crucial role in managing pelvic organ prolapse by providing conservative and non-surgical treatment options. The main focus is on strengthening the pelvic floor muscles, improving overall pelvic support, and providing strategies to manage symptoms. Here are some physiotherapy techniques commonly used for pelvic organ prolapse:
Also Read: 10 Gentle Workouts to Help Lower Back Pain at Home
A. Pelvic Floor Muscle Exercises
Specific exercises targeting the pelvic floor muscles can help improve their strength and tone, providing better support for the pelvic organs. A physiotherapist can guide you in performing these exercises correctly and developing a tailored program to address your specific type and severity of prolapse.
B. Pelvic Floor Muscle Training
In addition to exercises, pelvic floor muscle training may involve learning how to coordinate and engage the muscles effectively during daily activities, such as lifting, coughing, or sneezing. This can help reduce the strain on the pelvic floor and minimize the risk of prolapse worsening.
C. Postural Education
Maintaining good posture and body mechanics is crucial in managing pelvic organ prolapse. A physiotherapist can provide guidance on proper body alignment, lifting techniques, and strategies to avoid activities that increase intra-abdominal pressure.
D. Pessary Fitting and Management
A pessary is a removable device that can be inserted into the vagina to provide support for the pelvic organs. Physiotherapists with expertise in pelvic floor health can assess and fit the appropriate pessary for you. They can also provide education on proper use, cleaning, and ongoing management.
E. Lifestyle Modifications
Lifestyle changes can contribute to the management of pelvic organ prolapse. This may include maintaining a healthy weight, adopting proper bowel habits, managing chronic coughing, and avoiding activities that put excessive strain on the pelvic floor.
F. Education and Self-care
A physiotherapist specializing in pelvic floor rehabilitation can provide valuable education about pelvic organ prolapse, its causes, and strategies for self-care. This may include guidance on appropriate exercises, symptom management techniques, and long-term strategies for maintaining pelvic floor health.

It’s important to note that physiotherapy may not reverse severe cases of pelvic organ prolapse. In such cases, surgical intervention may be necessary. However, physiotherapy can play a vital role in managing symptoms, improving muscle strength and coordination, and even preventing the progression of prolapse in mild to moderate cases.
Remember, seeking the guidance of a qualified physiotherapist with expertise in pelvic floor rehabilitation is essential to develop a personalized treatment plan tailored to your specific needs. With their assistance, you can effectively manage pelvic organ prolapse and improve your overall pelvic floor health, allowing you to lead a more comfortable and active life.
3. Pelvic Pain
Pelvic pain is a complex and often debilitating condition that can affect both men and women. It refers to pain felt in the pelvic region, which includes the lower abdomen, pelvis, and perineum. Pelvic pain can have various causes, such as musculoskeletal dysfunction, nerve irritation, inflammation, or previous injuries. It may be acute or chronic, and the intensity and nature of the pain can vary.
Also Read: 5 Quick Home Remedies for Leg Cramp Relief and Prevention
Common Causes of Pelvic Pain
A. Pelvic Floor Muscle Dysfunction
Tension or dysfunction in the pelvic floor muscles can contribute to pelvic pain. This can occur due to muscle imbalances, spasms, trigger points, or weakness in the pelvic floor muscles. Musculoskeletal issues such as myofascial pain syndrome and pelvic floor muscle hypertonia can also lead to pelvic pain.
B. Endometriosis
Endometriosis is a condition in which the tissue that normally lines the uterus grows outside the uterus, leading to inflammation and pain. It can cause chronic pelvic pain, painful periods (dysmenorrhea), and pain during intercourse (dyspareunia).
C. Interstitial Cystitis/Bladder Pain Syndrome
This condition involves chronic inflammation of the bladder, resulting in pelvic pain, urinary urgency, and frequency. Pain may worsen with bladder filling and improve after urination.
D. Pelvic Inflammatory Disease (PID)
PID is an infection of the female reproductive organs, usually caused by sexually transmitted infections. It can cause pelvic pain, along with other symptoms such as fever, abnormal vaginal discharge, and painful intercourse.
E. Irritable Bowel Syndrome (IBS)
IBS can cause abdominal pain, bloating, and changes in bowel habits. The pain associated with IBS can sometimes radiate to the pelvic region.
Physiotherapy for Pelvic Pain
Physiotherapy plays a vital role in the management of pelvic pain by addressing the underlying causes and providing effective pain relief strategies. Here are some techniques commonly used in physiotherapy for pelvic pain:
A. Manual Therapy
Physiotherapists trained in pelvic health can use manual therapy techniques, such as myofascial release, trigger point release, and soft tissue mobilization, to alleviate muscle tension, reduce trigger points, and improve tissue flexibility in the pelvic region.
B. Relaxation Techniques
Chronic pelvic pain can be influenced by increased muscle tension and stress. Physiotherapists can teach relaxation techniques, such as deep breathing, progressive muscle relaxation, and mindfulness, to help reduce overall tension and promote pain relief.
C. Pelvic Floor Muscle Relaxation
In cases where pelvic pain is associated with pelvic floor muscle hypertonia or spasms, physiotherapists can guide individuals in techniques to relax and release the pelvic floor muscles. This may involve diaphragmatic breathing, gentle stretching, and relaxation exercises.
D. Biofeedback and Electrostimulation
Biofeedback and electrostimulation can be useful techniques in pelvic pain management. Its provides visual or auditory feedback on muscle activity, allowing individuals to become aware of and control their pelvic floor muscles. Electrostimulation uses low-intensity electrical currents to help relax and retrain the pelvic floor muscles.
E. Education and Lifestyle Modifications
A physiotherapist can provide education on pain management strategies, ergonomic modifications, and lifestyle adjustments to minimize triggers and promote pelvic health. This may include guidance on posture, proper body mechanics, bladder and bowel habits, and dietary modifications.
F. Collaborative Approach:
Physiotherapists often work in collaboration with other healthcare professionals, such as gynecologists, urologists, and pain specialists, to ensure a comprehensive approach to pelvic pain management. This interdisciplinary approach can provide a more holistic and effective treatment plan.

Remember, each case of pelvic pain is unique, and treatment approaches may vary. It is essential to consult a qualified physiotherapist specializing in pelvic health to receive an accurate diagnosis and develop an individualized treatment plan. By addressing the underlying causes of pelvic pain and implementing targeted physiotherapy interventions, you can experience significant relief and improved quality of life.
4. Pre and Postnatal Care
Pregnancy and childbirth are transformative experiences in a woman’s life, but they can also bring about changes and challenges, particularly in the pelvic floor. Pre and postnatal physiotherapy care focuses on promoting optimal pelvic health during pregnancy, preparing the body for childbirth, and facilitating postpartum recovery. It addresses common pelvic floor issues that arise during and after pregnancy, empowering women to have a positive and comfortable experience.
Preventive Care during Pregnancy
During pregnancy, the body undergoes significant changes to accommodate the growing baby. These changes can put strain on the pelvic floor muscles and lead to various Pelvic Floor Issues. Physiotherapy plays a proactive role in promoting pelvic health during pregnancy by:
A. Pelvic Floor Muscle Strengthening
Physiotherapists guide women through appropriate pelvic floor exercises to strengthen the muscles that support the bladder, uterus, and rectum. Strong pelvic floor muscles provide better support for the growing uterus, help prevent urinary incontinence, and contribute to overall pelvic stability.
B. Education on Body Mechanics and Posture
Physiotherapists provide guidance on maintaining proper posture, body mechanics, and ergonomic techniques during daily activities. This helps reduce strain on the pelvic floor and minimizes the risk of developing pelvic pain or dysfunction.
C. Pelvic Girdle Pain Management
Pelvic girdle pain is a common condition during pregnancy, causing pain in the pelvic area and lower back. Physiotherapists can provide techniques to alleviate discomfort, such as manual therapy, exercises, and advice on using support belts or braces.
D. Preparation for Labor and Delivery
Physiotherapy can help prepare the body for labor and delivery by teaching relaxation techniques, breathing exercises, and optimal positions for labor. This preparation aims to enhance pelvic floor function, promote effective pushing during delivery, and minimize the risk of perineal trauma.
Postnatal Rehabilitation
Postpartum physiotherapy plays a crucial role in supporting women’s recovery after childbirth and addressing any pelvic floor issues that may have arisen. The goals of postnatal care include:
A. Pelvic Floor Rehabilitation
Physiotherapists assess the pelvic floor muscles postpartum and provide appropriate exercises to regain strength, tone, and coordination. This helps prevent or address issues like urinary incontinence, pelvic organ prolapse, and perineal pain.
B. Diastasis Recti Rehabilitation
Diastasis recti is a separation of the abdominal muscles that can occur during pregnancy. Physiotherapy can guide women through exercises to help close the gap and restore core strength and stability.
C. Scar Management
For women who have undergone cesarean section or perineal tear/episiotomy, physiotherapists can provide scar management techniques, such as massage and gentle stretching, to promote tissue healing and reduce discomfort.
D. Posture and Body Mechanics
Physiotherapists address postural imbalances that may have developed during pregnancy and provide guidance on proper body mechanics for daily activities, such as lifting, carrying the baby, and breastfeeding. This helps prevent strain on the pelvic floor and promotes overall musculoskeletal health.
E. Return to Exercise
Physiotherapists guide women through a gradual return to exercise after childbirth, considering individual factors such as healing progress, pelvic floor strength, and overall fitness. This ensures a safe and effective transition back to regular physical activity.
F. Breastfeeding Support
Physiotherapists can offer ergonomic advice and positions to support optimal breastfeeding posture and help prevent neck, back, and shoulder pain.

By seeking pre and postnatal physiotherapy care, women can proactively address pelvic floor issues, optimize recovery, and improve overall well-being during this transformative phase of their lives. Physiotherapy provides guidance, support, and evidence-based interventions to promote pelvic health and empower women to thrive during pregnancy and beyond.
5. Sexual Dysfunction
Sexual dysfunction refers to difficulties or problems experienced by individuals that interfere with their sexual satisfaction and overall sexual well-being. It can affect both men and women and may have physical, psychological, or relational causes. Pelvic floor dysfunction can contribute to sexual dysfunction, as the pelvic floor muscles play a crucial role in sexual function. Physiotherapy can be a valuable approach to address and manage pelvic floor-related sexual dysfunction.
Common Types of Pelvic Floor-Related Sexual Dysfunction
A. Dyspareunia
Dyspareunia refers to pain or discomfort experienced during sexual intercourse. It can result from various factors, including pelvic floor muscle tension, scar tissue, hormonal changes, vaginal dryness, or psychological factors. Physiotherapy can help address the underlying pelvic floor issues and provide strategies for pain management.
B. Vaginismus
Vaginismus is a condition characterized by involuntary muscle contractions in the Pelvic Floor Issues, causing tightness and pain during attempted vaginal penetration. Physiotherapy techniques, such as pelvic floor relaxation exercises, desensitization techniques, and education on sexual response, can be beneficial in managing vaginismus.
C. Erectile Dysfunction (ED)
While erectile dysfunction is primarily a male sexual dysfunction, it can have an impact on both partners. Pelvic floor muscle dysfunction, including muscle weakness or hypertonicity, can contribute to ED. Physiotherapy interventions, such as pelvic floor muscle training and relaxation techniques, may be helpful in managing ED.
D. Decreased Sexual Desire
Pelvic floor dysfunction, hormonal changes, pain, and psychological factors can all contribute to a decrease in sexual desire. Physiotherapy can address pelvic floor-related concerns and provide strategies for pain reduction and overall sexual well-being.
Physiotherapy Approaches for Sexual Dysfunction
A. Pelvic Floor Assessment
A thorough pelvic floor assessment by a trained physiotherapist specializing in pelvic health is essential to identify any muscle imbalances, tension, weakness, or scar tissue that may contribute to sexual dysfunction. This assessment helps guide the development of an individualized treatment plan.
B. Pelvic Floor Muscle Training
Strengthening and coordination exercises for the pelvic floor muscles can be beneficial in improving muscle function and reducing tension. A physiotherapist can guide individuals through specific exercises and provide feedback to ensure proper engagement of the pelvic floor muscles.
C. Relaxation Techniques
Relaxation exercises and techniques play a crucial role in managing pelvic floor-related sexual dysfunction. These techniques help release muscle tension, reduce anxiety, and promote a more relaxed and pleasurable sexual experience.
D. Sensory Desensitization
In cases where pain or hypersensitivity is a contributing factor to sexual dysfunction, physiotherapists can guide individuals through desensitization techniques to gradually increase comfort and tolerance to touch or penetration.
E. Communication and Education
Physiotherapists play a vital role in providing education and guidance on sexual health, anatomy, and sexual response. They can facilitate open communication between partners and address any misconceptions or concerns related to sexual function.
F. Collaborative Care
In cases where psychological or relationship factors contribute to sexual dysfunction, a collaborative approach involving a physiotherapist, sexual therapist, or mental health professional may be beneficial to address all aspects of the issue.

It’s important to note that sexual dysfunction can have multiple causes, and physiotherapy may be one part of a comprehensive treatment plan. Consulting with a qualified physiotherapist specializing in pelvic health will ensure a thorough assessment and the development of an individualized treatment approach tailored to your specific needs. By addressing pelvic floor-related factors and implementing appropriate interventions, individuals can experience improvements in sexual function and overall sexual well-being.
Conclusion
Pelvic floor issues can have a significant impact on one’s quality of life, but with the help of physiotherapy, effective solutions are within reach. Whether you are dealing with urinary incontinence, pelvic organ prolapse, chronic pelvic pain, or sexual dysfunction, seeking the expertise of a physiotherapist can provide valuable guidance and support. With tailored exercises, education, and a holistic approach, physiotherapy can help strengthen the pelvic floor, alleviate symptoms, and improve overall well-being. Take the first step towards a healthier pelvic floor and regain control of your life by consulting a physiotherapist today.
Tags:
- Common Pelvic Floor Issues,
- How Physiotherapy Can Help,
- Internal Pelvic Floor Therapy,
- Pelvic Floor,
- Pelvic Floor Issues,
- Pelvic Floor Physical Therapy,
- Pelvic Floor Physical Therapy Near Me,
- Pelvic floor physiotherapy,
- Pelvic Floor Physiotherapy Clinic,
- Pelvic Floor PT Near Me,
- Pelvic Floor Therapy,
- Pelvic Floor Therapy Near Me,
- Physiotherapy Approaches for Sexual Dysfunction,
- Physiotherapy for Pelvic Organ Prolapse,
- Physiotherapy for Pelvic Pain,
- Physiotherapy for Urinary Incontinence,
- Postnatal Rehabilitation,
Recent Posts
All Categories
- Acupuncture
- Arthritis
- Back Pain
- Chiropractic
- Chronic Pain
- Cupping Therapy
- Exercise
- Fibromyalgia
- Hamstring Pain
- Headaches
- Health
- Injury Clinic
- Joint Pain
- K Taping Therapy
- Knee pain
- Laser Therapy
- Manual Therapy
- Massage Therapist
- Massage Therapy
- Mental Health
- Motor Vehicle Accident
- Neck Pain
- Nerve pain
- Orthotics
- pelvic floor physiotherapy
- Physiotherapy
- Sciatica Pain
- Scoliosis Exercises
- Shockwave Therapy
- Shoulder pain
- Sports Physiotherapy
- VRT
- 905-846-4000
- 905.846.2100
- Kennedy Road & Sandalwood Road Unit#1, 170 Sandalwood Prky East Brampton, ON. L6Z 1Y5
MALTON
- 905-364-3900
- 905.676.9499
- Airport Road & Drew Road Unit# 139, 2960 Drew Rd. Mississauga, ON L4T 0A5
ORANGEVILLE
- 519-217-9300
- 519.217.9588
- Hwy 9 & Rolling Hills Drive Unit #4 , 50 Rolling Hills Drive Orangeville, ON L9W 4W2


Leave a Comment